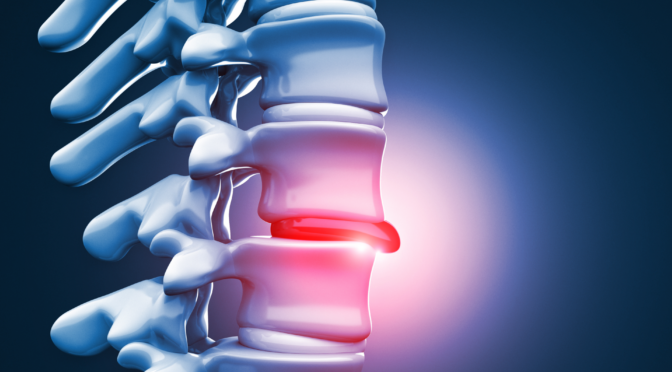
Herniated Disc
Let’s start by understanding what a disc is. A disc is a spongy cushion that separates the bones in your spine. Discs act as shock absorbers for your body in everyday movement.
When this disc has a problem, you’re suffering from a herniated disc. Here, the disc could have slipped from its position. Alternatively, the jellylike substance that forms its interior could be seeping out through a tear, also referred to as a ruptured disc.
Signs & Symptoms
In the early stages, a herniated disc may not show any symptoms. With time, you will begin to experience some discomfort, depending on the location of the disc. Although this condition can affect any part of the spine, it mainly occurs in the lower back. The pain and discomfort from the faulty disc often extend beyond the affected area, an indicator that the slipped disc could be pressing on some nerves.
The most common symptoms include pain, numbness, and a tingling sensation on and around the affected area. A cervical disc herniation affects the upper back, causing pain in your shoulders, arms, and neck. If the pain is in the lower back, chances are you’re dealing with a lumbar disc herniation, which could cause pain in your buttocks, thighs, and legs.
Common Triggers
What causes disc herniation? While some discs slip or rupture due to an excessive force such as a fall or lifting heavy objects, most disc problems are age related. As you get older, the gradual wear and tear cause disc degeneration, making it more vulnerable to damage. That said, certain factors increase the risk of suffering from this condition, such as:
- Genetics
- Excess weight, which exerts pressure on the discs
- Physically demanding jobs that cause strain to the spine
- Regular driving (the sitting position coupled with vibrations)
- Sedentary lifestyle
- Smoking
Diagnosis
Disc herniation diagnosis occurs in several ways, starting with a physical test where the doctor checks the affected area for tenderness. You may need to perform simple exercises such as stretching, bending, twisting, or walking to help narrow down the source of the pain.
In mild cases, a physical test is enough for a diagnosis. If the disc herniation seems to have pressed on the nerves, you’ll need to undergo an imaging test, such as:
- MRI
- CT scan
- Myelogram
- X-ray
Nerve tests can also help determine the location and extent of the nerve damage.
Treatment
Depending on the severity of your condition, the doctor will decide on the treatment option that best suits you, which can be one or a combination of the following:
- Physical Therapy
Therapy can help with mild cases, where the doctor guides you on exercises that reduce pain and ease mobility.
- Medication
A prescription of pain relievers will reduce discomfort. Medication differs depending on the intensity of your pain.
- Injections
Injections with a steroid can calm the nerve down and decrease some of the swelling. This can relief pain anywhere from a couple hours to months.
- Surgery
Surgery is an option if your condition does not improve with the above treatments. Here, doctors may remove the bulging section of the disc, relieving the pressure on the spinal canal
OFFICE HOURS
Monday: 8 AM - 4:30 PM
Tuesday: 8 AM - 4:30 PM
Wednesday: 8 AM - 4:30 PM
Thursday: 8 AM - 4:30 PM
Friday: 8 AM - 4:30 PM
Saturday: Closed
Sunday: Closed
PROFESSIONAL DOCTORS
Dr. Schell has designed surgical techniques now used by many spinal surgeons.
MODERN EQUIPMENT
The most up-to-date medical equipment, to give you the best care that you deserve.
Professional spinal care and pain care experts are standing by to assist you. If we are not able to answer your question without an on-site appointment, we can schedule one for you.